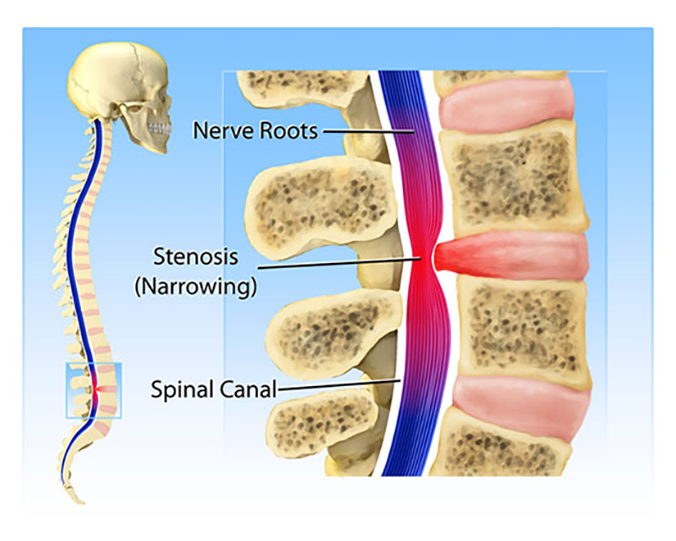
Almost every chronic back pain condition is extremely unpleasant, but one of the most excruciating is spinal stenosis. Spinal stenosis is especially painful because it involves direct pressure to the nerves in the spinal column. This condition is related to a narrowing of the spinal canal—the space in the spine where the nerve fibers are located.
Spinal stenosis is most often associated with osteoarthritis, a condition in which the cushiony cartilage between bones break down. This allows the spinal vertebrae to directly contact one another and erode the bone. Over time, this can lead to the creation of bony growths called bone spurs which narrow the spinal canal and pinch the nerves.
Spinal stenosis is a relatively common chronic pain condition. There are between 250,000 and 500,000 Americans with spinal stenosis. It is most common in people aged 30 to 50, with men twice as likely to have this condition than women.
There are many pain management techniques for spinal stenosis, depending on the exact cause and severity of the condition. These may range from mild pain relief medications to physical therapy and, even, surgical intervention. Upon diagnosis, your physician will detail all of the available pain management treatment options along with their potential benefits and risks.
What Is Spinal Stenosis?
Stenosis is a general term that describes the narrowing of any channel in the body, and spinal stenosis refers to any shrinkage of the canal in the spine that houses the nerves. Thirty-one sets of nerves from the limbs and trunk of the body join the spinal nerve fiber by traversing small openings in the spinal canal found between the vertebrae.
In some cases, an injury or illness may cause one of these openings called neuro-foramen or the spinal canal itself to shrink. In turn, this may apply pressure on the nerves and induce pain, numbness or improper function.
Recognizing the Symptoms
Spinal stenosis may not be easy to identify because it may appear in the neck (cervical spine), upper back (thoracic spine), or lower back (lumbar spine). Although neck or back pain may be one of the symptoms of spinal stenosis, it may not be the primary symptom. Other symptoms include
- Numbness or tingling in limb
- Difficulty walking or remaining upright
- Neck or back pain
- Weakness in arm, leg, hand or feet
- Bowel or bladder dysfunction
You should see a doctor as soon as possible if you experience any of these symptoms. If your doctor suspects spinal stenosis, then they may order one or more of the following tests to confirm the prognosis:
- X-ray—this test may have less resolution than other tests, but it may provide broad confirmation of osteoarthritic bone spurs.
- MRI—a magnetic resonance imaging scan can produce a detailed cross-sectional picture of your spine, allowing your doctor to see if the spinal canal has narrowed and is impinging upon the spinal nerves.
- CT scan—a computerized tomography scan uses contrast dyes and X-ray imaging to provide a detailed image of the spine. A CT scan may identify herniated discs, bone spurs or tumors that are pressing upon the spinal nerve.
Causes of Spinal Stenosis
There are many health conditions which may cause the spinal canal to shrink, so it may take some time and effort to pinpoint the exact condition. These may include
- Osteoarthritis—the most common cause of spinal stenosis is osteoarthritis. Osteoarthritis degrades the cartilage in joints which allows bones like the spinal vertebrae to rub against one another. The friction creates bone spurs that push into the spinal canal or neuro foramen (openings where nerves enter the spinal canal).
- Bulging disc—between the vertebrae are cushions called discs. Sometimes these discs may be dislodged or torn, and a part may bulge out from the vertebrae. This extruded tissue may press against a nerve bundle causing pain or dysfunction.
- Paget’s disease—this illness causes your body to create bone faster than is normal. In healthy people, new bone is created to replace old tissue, but those affected by this illness, instead, accumulate new bone which can extrude into the neuro-foramen or spinal canal.
- Injury—if you experience trauma to your spine, there may be dislocations or bone fractures that impinge upon spinal nerves. Even if there is no structural malformation, an injury may cause damaged tissue to swell and press on nearby nerves.
- Cancerous growth—in rare cases, cancer may originate or spread to the spine. A tumor may press upon a spinal nerve and produce symptoms of spinal stenosis.
Spinal Stenosis Treatments
Depending on the cause of the spinal stenosis and the severity of the symptoms, there may be one or more pain management treatment options. Your doctor may recommend one of the following:
- Lifestyle changes—depending on the activities that you typically engage in, your doctor may ask you to limit certain activities or adopt new ones that promote pain mitigation. For example, if your stenosis is found in your lower back, your doctor may recommend less sitting at a desk or driving. Your doctor may also urge you to take up a more active lifestyle or eat a healthier diet.
- Pain relievers—if you experience pain regularly, you may be put on a medication regimen. In most cases, your doctor will probably prescribe over-the-counter drugs like Tylenol or Advil which are quite effective at pain management. If you encounter severe or chronic pain, more powerful pain killers may be employed, but usually only for short periods.
- Epidural injections—if your pain doesn’t respond to more conventional forms of treatment, you may be a candidate for epidural injections. This procedure involves injecting a corticosteroid near the spinal stenosis site so that swelling will come down.
- Surgery—as a last resort, your doctor may recommend a surgical option. If the location and cause of the stenosis is precisely identified, a surgeon may use one or more decompression procedures to relieve pressure. These options may include a disc replacement, discectomy or a laminectomy.
- Superion – another option for treating spinal stenosis, Superion implants act as an indirect decompression device. Its anatomic design provides optimal fit and preserves a patient’s anatomy and ability to maintain motion. Superion acts as an extension blocker, relieving pressure on the affected nerves in the manner that one would achieve relief in a seated or flexed position. Available in multiple sizes to accommodate varying patient anatomy, Superion ensures controlled movement and minimizes post-procedure complications. Superion was developed to provide patients with a safe and effective alternative when conservative treatment has failed and laminectomy is too aggressive.
Article written by: Dr. Robert Moghim – CEO/Founder Colorado Pain Care
M.D. Disclaimer: The views expressed in this article are the personal views of Robert Moghim, M.D. and do not necessarily represent and are not intended to represent the views of the company or its employees. The information contained in this article does not constitute medical advice, nor does reading or accessing this information create a patient-provider relationship. Comments that you post will be shared with all visitors to this page. The comment feature is not governed by HIPAA and you should not post any of your private health information.



