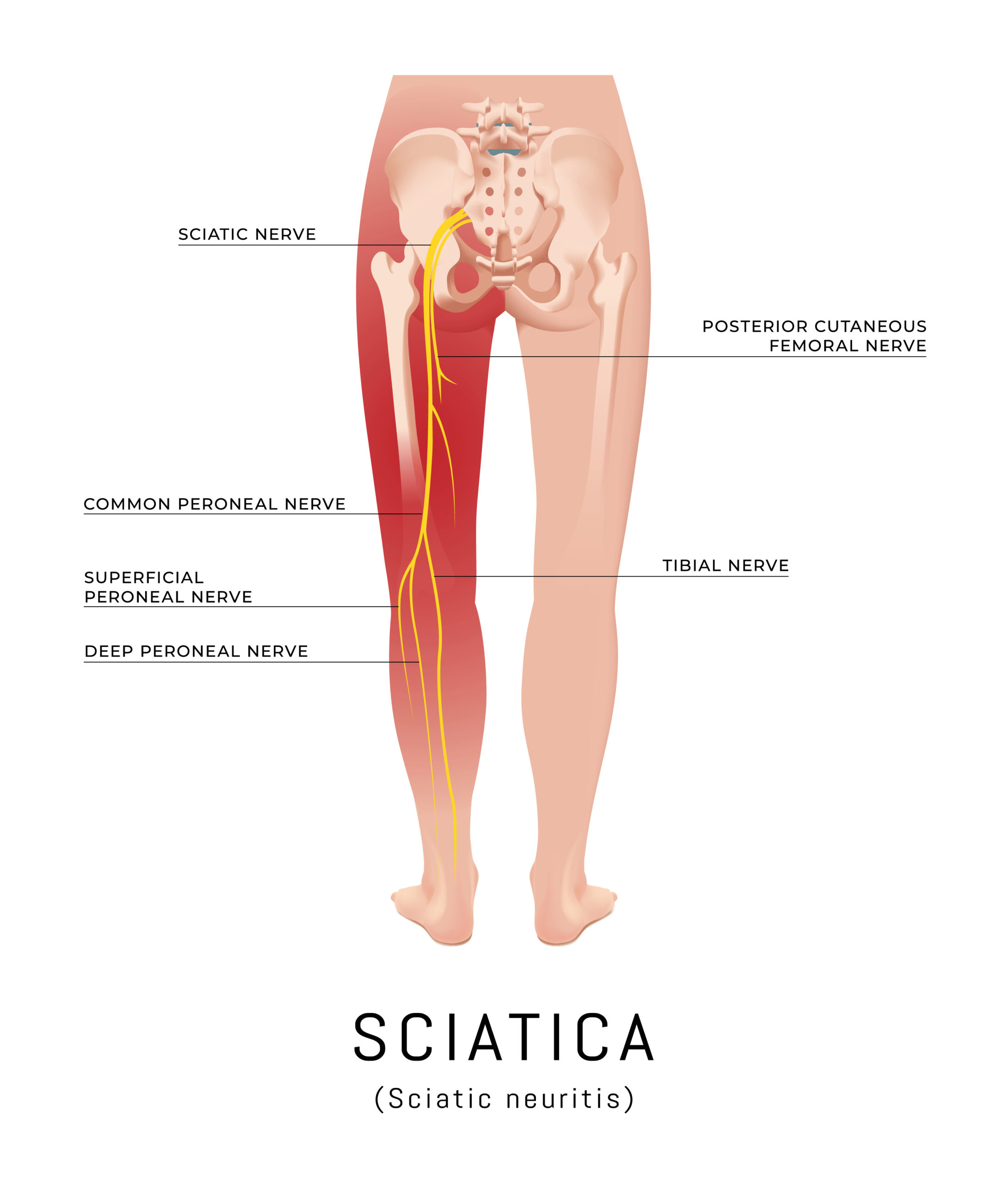
Home Remedies for Sciatica
Sciatica can be an extremely painful health condition, but you should be happy to know that, in most cases, this condition resolves in a few weeks. Sciatica usually presents with pain, inflammation or numbness in the lower back and legs; this may be caused by a herniated spinal disk, bone spur or spinal stenosis (narrowing of the spinal passage) that puts pressure on the sciatic nerve. The sciatic nerve, which is the largest nerve in the body, originates in the lumbar region of the spine and travels down to the feet.
Sciatica is one of the most common pain conditions with as many as 40 percent of the population experiencing it at some point in their lives. Among the risk factors for developing sciatica are obesity, tobacco use, and sedentary lifestyle.
A Closer Look at Sciatica
Most people who encounter sciatica assume it is a back pain condition, but this is not strictly true. The sciatic nerve does originate in the lower back, but because the nerve extends down to the feet, symptoms may not be localized to the back.
In general, sciatica may present wildly differently from episode to episode. Some may involve numbness, tingling, burning or stabbing pain, and the intensity of symptoms may sometimes be mild while other times almost debilitating.
What is surprising in many, if not most, sciatica cases is that there is usually no injury that sets off the condition. In most sciatica cases, the condition is caused by years of sitting or bending over which causes a spinal disc to rupture or a vertebra to misalign and pinch the sciatic nerve. Osteoarthritis may play a strong role in the development of sciatica.
Diagnosing Sciatica
The primary method of diagnosing sciatica is via medical history and physical examination. One of the hallmarks of sciatica is radiating pain that extends from the lower back to the lower legs. Although there may be some back pain symptoms, it is usually less severe than the leg pain.
The most commonly used diagnostic test is the straight leg raise. During this test, your clinician will raise each leg individually while you lie on your back. The clinician will determine the nature of your condition, i.e. sciatica or a generalized back pain, by noting when the discomfort occurs during the test. If the patient indicates pain while the leg is from 30 to 70 degrees above the plane, and this pain is expressed in the leg as well as the back, there is a high level of confidence that this is sciatica.
Treating Sciatica
Most occurrences of sciatica will disappear on its own in a few hours or days, but there are episodes which may go on for weeks or months. Most sciatica cases can be treated with self-care, but there are some extreme cases in which symptoms interfere with movement or daily activities and necessitate surgical intervention.
If you experience sciatica-like symptoms, then you should visit your doctor who can confirm the diagnosis and possibly identify the underlying structural issue. In most circumstances following a sciatica diagnosis, your physician will recommend one or more of the following home treatment options:
- Back exercises—it may go against your instincts to engage in physical activity while your back or legs hurt, but low-impact exercises like water aerobics, stationary biking and yoga can be quite effective at reducing symptom severity and strengthening your back to prevent future back issues. Stronger back muscles also help support the spine and alleviate pressure on spinal nerves which can reduce the frequency and intensity of sciatica episodes.
- Stretching—another form of physical activity that may alleviate sciatica symptoms is stretching. Stretching should be performed slowly and gently; stop immediately if you notice any pain. You may try pulling your knees up to your chest, seated hip stretch or seated spinal twist. The purpose of these stretches is to loosen the buttocks, hamstrings and calves which can exert pressure on the sciatic nerve.
- Heat and cold therapy—Ice and heat can alleviate many of the symptoms that accompany sciatica and accelerate the healing process. Applying ice for 15 minutes can numb the affected area, while heat will increase blood flow and improve healing. These applications can also reduce muscle spasms which are common among sciatica patients.
- Sit up straight—if you work at a desk or in a bent position for much of the day, pay close attention to your posture. You should try to sit with your head aligned with your hips. You should also take frequent breaks from sitting to relieve strain on your spine.
- Non-steroidal anti-inflammatory drugs–non-steroidal anti-inflammatory drugs or NSAIDs like Tylenol and Advil can provide significant pain relief because they reduce inflammation, a common feature of herniated spinal discs. Prior to taking NSAIDs, you should discuss them with your doctor because there are some important side effects like stomach irritation.
- Steroid injections—certain sciatica patients may benefit from steroid injections at the site of their herniated disc. Steroids relieve pain and other sciatica symptoms by reducing swelling of the spinal disc and surrounding tissue.
Surgical Options
For about 5 to 10 percent of sciatica patients who do not respond to more conservative therapies, there is the option of having a surgical procedure. This is typically reserved for patients whose condition does not improve after three months or there is loss of bladder or bowel control.
There are two types of surgeries for sciatica:
- Diskectomy—this kind of surgery involves removal of the part of the spinal disk or bone that is pressing on the sciatic nerve. Usually, only a small part of the impinging disk is cut away, but it can be necessary to remove the entire disk.
- Laminectomy—this procedure removes part of the lamina which is the bone surrounding the spinal cord. This should alleviate the pressure on the sciatic nerve caused by spinal stenosis. This is a more involved operation than a discectomy and may require a hospital stay of one or two days.
Article written by: Dr. Robert Moghim – CEO/Founder Colorado Pain Care
M.D. Disclaimer: The views expressed in this article are the personal views of Robert Moghim, M.D. and do not necessarily represent and are not intended to represent the views of the company or its employees. The information contained in this article does not constitute medical advice, nor does reading or accessing this information create a patient-provider relationship. Comments that you post will be shared with all visitors to this page. The comment feature is not governed by HIPAA and you should not post any of your private health information



