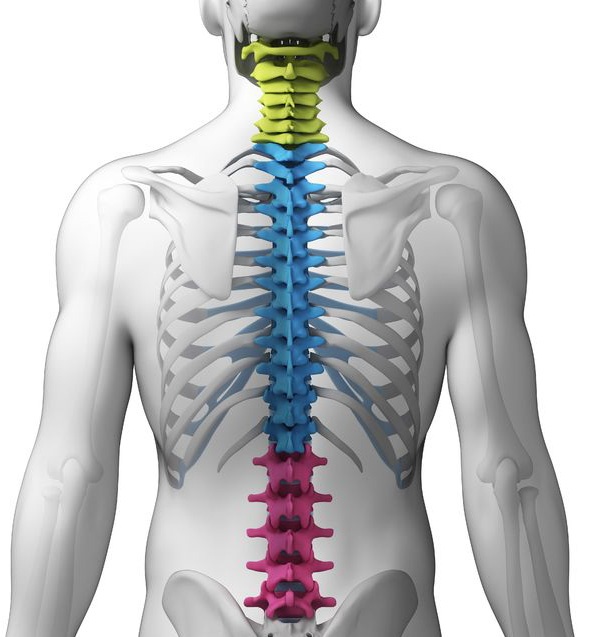
Your spine is the central support for your trunk, neck and head. As a result, it plays a critical role in maintaining bodily architecture, conveying neural impulses to and from the brain, and anchoring key musculature. Because it plays so many important roles in physiological function, any problems involving the spine can be challenging to identify and remedy.
One of the most painful and problematic spine conditions is spinal compression fractures. Spinal compression fractures are breakages of the spinal vertebrae (bones that make up the spinal column). They often result from weakened bone caused by osteoporosis. Spinal compression fracture symptoms may be triggered by bending down and forward.
Although most spinal compression fractures resolve eventually on their own, they can result in diminished height and a humped back. There are a variety of pain management techniques if severe or lingering pain is the primary compression fracture symptom. There are also some surgical options available to stabilize the spine.
A spinal compression fracture is a relatively common occurrence, especially among seniors. Almost 1.5 million spinal compression fractures occur annually in the U.S., and almost a quarter of all post-menopausal women will experience one during their lifetime.
Why Is the Spine So Vulnerable?
The spine is a strong but complex structure composed of 24 bony vertebrae. Each of these bones is connected to other bones and muscles via ligaments and tendons. Furthermore, the 24 vertebrae are designed to house and protect the spinal cord, the primary neural pathway from the brain. There are spaces in each vertebra that allow the spinal cord to traverse its length as well as allow nerves to connect with it.
Each of the bones—as well as the joints between them—of the spine serves a variety of crucial functions. As we age, the bone as well as the connective tissue between them often degrade. If a vertebra weakens and is exposed to undue pressure, there is a high probability that one of these bones could fracture.
Spinal Compression Fracture Symptoms
Although most people think of a bone fracture as an explosive event, in many cases, a spinal compression fracture may occur gradually over time. Compression fracture symptoms usually start with tiny cracks in the bone that produce back pain. Eventually, if fracturing spreads, the entire vertebra will collapse. Most patients that exhibit spinal compression fractures usually see breakages in the front part of the vertebrae, where the bone is weaker.
Other symptoms include:
- Worsening pain while walking or standing
- Difficulty bending or twisting at the waist
- Lost height
- Arched back
- Digestion issues including constipation, diminished appetite or weight loss
- Hip pain
- Difficulty breathing
In some cases, someone with a spinal compression fracture may not feel any pain at all; for others, this pain may be mild. Among select patients, this pain caused by spinal compression may be chronic.
Diagnosing Spinal Compression Fractures
Almost two-thirds of patients with spinal compression fractures are never properly diagnosed because they consider back pain merely a side effect of aging. Even for many seasoned physicians, it can be difficult to distinguish between a spinal compression fracture and other common health conditions like arthritis or a muscle strain.
Although it may not seem like it, it is good news that spinal compression fractures are the most common symptom of osteoporosis. Almost 66,000 office visits and more than 45,000 hospital stays every year are related to spinal compression fractures. Because vertebral compression fractures occur so often, your physician is likely to check for it if you present with the following conditions
- Back pain that starts with lifting, position change, coughing or sneezing
- Lingering back pain that worsens over time
- Bulge in the vertebral area
- Pain that radiates to the legs
If your physician suspects that a spinal compression fracture has occurred, then they may order an X-ray, CT scan, MRI, or bone scan. Your physician may also recommend a bone density test to determine if your bones are weaker than normal. If your bone density is low, then this may prove problematic during healing and treatment.
How to Treat Spinal Compression Fractures
Depending on the type of spinal compression fracture symptoms you are experiencing and any relevant health conditions—especially your bone health—your doctor may recommend one or more of the following treatments.
- Bed rest—in many cases, a spinal compression fracture may heal on its own if given time. Many physicians may allow up to three months of non-intervention for the compression fracture symptoms to resolve independently. Most medical experts recommend only a few days of actual inactivity.
- Back brace—if your doctor thinks that the fracture can heal on its own, they may recommend a support device to keep your back rigid. Although a back brace will limit spinal movement so that bones can knit at an optimal pace, there is the risk of weakening back muscles which can raise the risk of other back conditions.
- Pain management—many patients expect their doctor to prescribe the most powerful pain relievers available for a spinal compression fracture, but most people find that they can manage their pain effectively with just over-the-counter drugs like aspirin or acetaminophen. If the pain is chronic and severe, your physician may prescribe opioid pain killers but only for limited periods of time.
- Vertebroplasty—this surgical procedure is minimally invasive and helps to stabilize a damaged vertebra. An X-ray-guided needle is inserted into the spine, and a bone cement compound is injected. This compound hardens in less than ten minutes, stabilizing the fractured bone, and most patients are able to return home that same day or the next day.
- Kyphoplasty—this surgical operation corrects bone deformations resulting from a spinal compression fracture. Like a vertebroplasty, a bone cement is used to secure a damaged vertebra, but this procedure uses a tiny balloon to create a space into which the compound is inserted.
- Spinal fusion surgery—if it is necessary to minimize motion between two or more spinal vertebrae, then doctors may use spinal fusion surgery. Plates or rods are usually inserted to keep parts of the spine rigid, limiting pain and compression.
Article written by: Dr. Robert Moghim – CEO/Founder Colorado Pain Care
M.D. Disclaimer: The views expressed in this article are the personal views of Robert Moghim, M.D. and do not necessarily represent and are not intended to represent the views of the company or its employees. The information contained in this article does not constitute medical advice, nor does reading or accessing this information create a patient-provider relationship. Comments that you post will be shared with all visitors to this page. The comment feature is not governed by HIPAA and you should not post any of your private health information.



