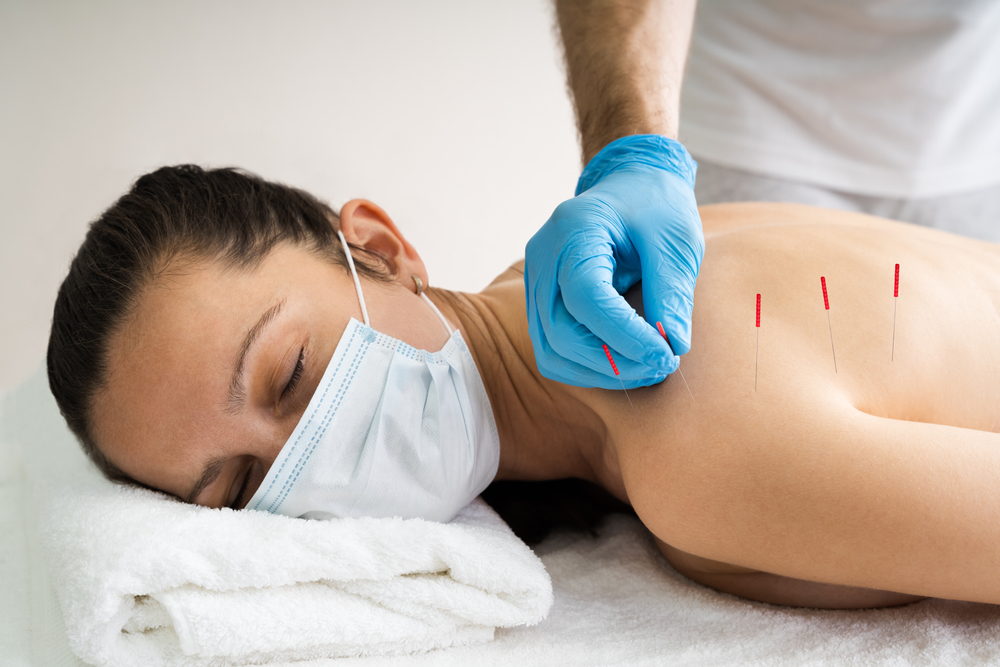
Dry Needling for Back Pain
Back pain is one of the most common health conditions with almost four in five people experiencing this condition at some point in their lives. Back pain is one of the most prevalent reasons for missed work and accounts for almost 264 million lost work days annually. This condition is the third leading cause for doctor’s visits and the number one cause of disability in the world.
Your back is a complex network of bones, muscles, connective tissue and nerves which may become dysfunctional due to illness or injury. There are a myriad of ways that back pain can originate including bulging discs, vertebral fracture or spinal stenosis, but one of the more common causes is myofascial pain. Myofascial pain may originate due to stress, poor posture or a muscle strain, but it manifests as muscle tension or knots.
An increasingly popular treatment for myofascial back pain is dry needling, a technique similar to acupuncture. Like acupuncture, dry needling involves the insertion of thin, sterile needles into the skin and upper levels of muscle. This helps tense muscles relax and boosts your body’s production of natural painkillers called endorphins.
A Brief History of Dry Needling
Unlike acupuncture which is based on Eastern medicine that endorses the existence of an energy flow through living things called chi, dry needling is founded on scientific evidence. Dry needling was developed in the 1940s by Dr. Janet Travell who identified muscle trigger points. Initially, Dr. Travell worked with “wet” needling, i.e. hypodermic needles that injected medications, but she soon discovered that she could achieve similar results with dry needles.
In the 1970s, there was a further refinement of dry needling. Dr. C. Gunn introduced Intramuscular Stimulation or IMS which identified the nerve root as the source of myofascial pain. Also during this period, Dr. H. C. Dung discovered the homeostatic points.
Modern Dry Needling Technique
When you begin your dry needling program, your physical therapist should first perform an in-depth evaluation that identifies key back pain issues and muscle groups along with their trigger points. This provides a broad framework for your physical therapist to work with.
Prior to insertion, the therapist will palpate the muscle which involves feeling around the affected muscle to identify the trigger point. This palpation may elicit a twitch response from the muscle if the trigger point is stimulated. The therapist will then place a howl glass tube over the trigger point which will guide the needle.
A very thin, stainless steel needle is then inserted into the hollow tube then pushed into the skin and underlying muscle. In most circumstances, there is only very minor discomfort. The needles may be manipulated by the physical therapist in an effort to stimulate a twitch response. Once inserted, the needles may remain in from 10 to 30 minutes.
Some patients may experience an immediate relaxation in the contracted muscle along with a reduction in pain symptoms and increase in range of motion. For others, it may take one or two days or even additional dry needling sessions to experience symptom relief.
Most physical therapists recommend that patients wait at least a few days between dry needling sessions. This allows you to recover from any soreness caused by the previous session.
Furthermore, it is important to continue other therapies for your myofascial back pain that your physical therapist may recommend. This may include strength and flexibility exercises, TENS, or ice and heat treatments. Dry needling is almost never used as a stand-alone therapy for back pain; a number of studies show that dry needling is most effective when used in concert with other therapies.
How Successful is Dry Needling in Treating Low Back Pain?
Despite being around for many decades, dry needling has only obtained widespread adoption by the medical community in recent years. That is why there is limited scientific research into its efficacy as a low back pain treatment, and the studies that have been performed are of low to middling reliability. To date, there have been no studies into this topic with broad test populations and unimpeachable testing standards.
One meta-review published in Medicine in 2018 analyzed 16 randomized controlled trials involving dry needling for low back pain. The study authors concluded that most of the trials had a high or unclear risk of bias, making them unsuitable as reliable scientific evidence. They did suggest that dry needling was more effective at low back pain relief than acupuncture. Dry needling was also more effective than sham needling at pain relief. It remains unclear if dry needling is better than other therapies like laser treatments or exercises in relieving low back pain.
Ultimately, whether dry needling works for you may depend on you. Although there are no conclusive studies supporting dry needling’s ability to relieve pain across a broad cross-section of low back pain sufferers, there is plenty of anecdotal evidence suggesting that dry needling has potent pain-relieving properties for at least some people. The only way to know if it will work for you is to try it.
Potential Risks Associated with Dry Needling
Most physicians will at least present the possibility of dry needling as a treatment for myofascial low back pain, even if they do not believe in its efficacy themselves. This is because dry needling has very few risks, and in most cases, those risks are exceedingly minor. Among those risks are
- Bleeding—for most people, there is likely to be only minimal blood loss at the site of needle insertion. However, for people with hemophilia or on blood-thinning medication, this could be more severe.
- Bruising—about 15 to 20 percent of people may experience bruising.
- Temporary pain—some 60 to 70 percent of people who participate in a dry needling session will experience some pain or soreness for a short period following it.
- Pneumothorax—in less than 0.01 percent of people, a serious condition called pneumothorax may occur. This condition is the result of a puncture of the chest wall, causing the lung to collapse.
Article written by: Dr. Robert Moghim – CEO/Founder Colorado Pain Care
M.D. Disclaimer: The views expressed in this article are the personal views of Robert Moghim, M.D. and do not necessarily represent and are not intended to represent the views of the company or its employees. The information contained in this article does not constitute medical advice, nor does reading or accessing this information create a patient-provider relationship. Comments that you post will be shared with all visitors to this page. The comment feature is not governed by HIPAA and you should not post any of your private health information.



