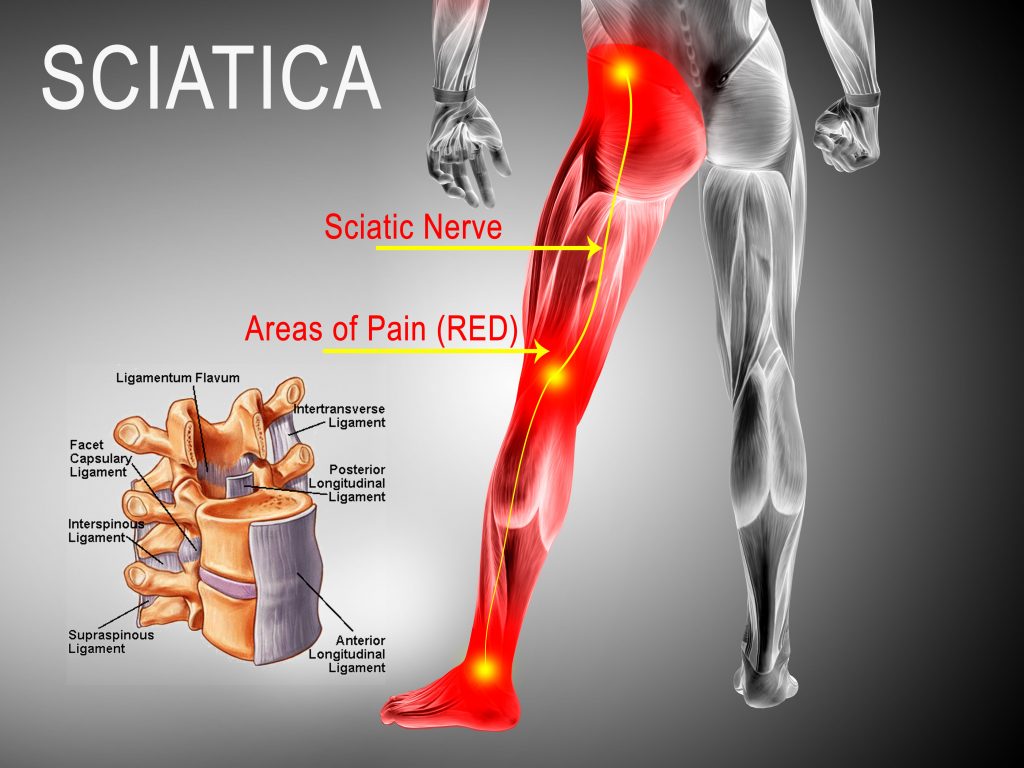
Back pain is one of the most disruptive forms of chronic pain, but some forms of back pain are more easily identified and treated than others. One of the most recognizable and treated is sciatica pain which is caused by pressure on the sciatic nerve. The most common cause of sciatica pain is a herniated disc in the lower back typically resulting from injury or age.
Sciatica pain can be intensely painful, but the good news is that this condition typically clears up in a few weeks. Only a limited number of patients require a surgical procedure to relieve the nerve pressure. If you experience sciatica pain in the buttocks of one leg along with any of the following symptoms, you should visit a doctor immediately:
- Pain is not diminished by non-surgical treatment
- Severe or debilitating pain
- Foot drop
- Impaired motor function
- Muscle weakness in a leg
- Any changes in bladder or bowel function
What Is Sciatica?
The sciatic nerve is the longest nerve in the human body and stretches from the lower back down both legs. Sciatica is an umbrella term that includes any pain or neurological symptoms affecting any part of this long nerve.
The most common physical cause of sciatica is a bulging disc in the lumbar region of the back. Between the spinal vertebrae are spongy discs that help cushion and support the spine. If there is an injury, then this disc may shift and press on the sciatic nerve. Also, over time, the tough exterior of the disc may degrade; consequently, the jelly like interior may extrude through tears and pinch the sciatic nerve.
Although pain in one side of the buttocks is the hallmark symptom of sciatica, this condition may also present with the following symptoms:
- Numbness
- Tingling
- Burning
- Prickling
Sciatica pain usually begins in the lower back and spreads down the thigh of one leg and into the lower leg and foot. Most patients characterize the pain as a burning, sharp or electrical sensation. The pain is often worse when standing or sitting still, and improves while lying or walking.
Non-surgical Treatments for Sciatica Pain
Most physicians recommend conservative therapies to initially treat sciatica back pain. Among the most commonly prescribed are
- Bed rest—in most circumstances, physicians do not recommend extended periods of bed rest. Although short periods of rest may be necessary after a sciatica back pain flare-up, you should remain as active as possible to promote healing and limit the risk of your condition progressing to a chronic one. Too much bed rest can weaken muscles needed to support the spine as well as dry out and harden spinal discs, making them more prone to damage. e
- Heat or ice therapy—the application of cold to numb the back pain and reduce swelling has prove quite effective for many sufferers. Short periods of icing—20 minutes or less—should be alternated with heat therapy which can also soothe pain, promote circulation and expedite healing.
- Anti-inflammatory medications—one of the key physiological responses to sciatica pain is inflammation of the surrounding tissue which can further aggravate pain symptoms. That is why many doctors recommend anti-inflammatory drugs like NSAIDS (e.g. aspirin, ibuprofen, naproxen) to help limit swelling. In some cases, your doctor may recommend steroid injections to help reduce inflammation and pain.
- Physical therapy—for many patients, physical therapy that includes stretches and back strengthening exercises can help alleviate sciatica back pain. These exercises can help stretch your back and reduce pressure on your sciatic nerve. They may also help align your spine in to a more natural and less painful posture. It is important to maintain your physical therapy regimen until your doctor tells you to stop so that you can obtain the maximum benefit.
- Exercise—one key factor for many sciatica pain patients is the presence of belly fat. Not only does this press on the spine, making you more prone to a herniated disc, but it may also exacerbate a sciatica condition by increasing pressure on the sciatic nerve. That is one of the primary reasons why you should maintain a regular exercise regimen that includes stretching, cardiovascular exercise, and muscle building exercise. Discuss any new fitness program with your doctor prior to beginning to prevent any injury.
- Pain relievers—one of the priorities of sciatica back pain treatment is managing pain symptoms, so your doctor should prescribe pain relievers immediately after diagnosis. Although the pain may be severe, most physicians recommend that sciatica back pain patients remain on over-the-counter pain medications initially; this is because OTC drugs may be as effective as prescription medications for many patients and many of these drugs have anti-inflammatory properties that help alleviate pain. If your pain does not respond to OTC drugs, then your doctor may prescribe opioids or muscle relaxants for short periods of time.
Surgical Treatments for Sciatica Pain
- Discectomy—this surgical procedure removes the part of the spinal disc or bone spur that is impinging upon the sciatic nerve. Although the goal is to cut away only the portion of bone or disc that is pressing, in some cases, surgeons may have to remove the entire disc. Many patients who undergo this procedure are able to return home the same day.
- Laminectomy—in this procedure, the lamina—the bony plate in the spinal canal—is removed. This lamina removal alleviates pressure on the sciatic nerve and mitigates pain and neurological symptoms.
Surgery, of course, comes with some serious risks, but some of these potential complications may be mitigated by new surgical techniques that use microscopic incisions and minimal invasive procedures. This allows you to be ambulatory within 24 hours, although you may still need 2 to 4 weeks to fully recover.
Article written by: Dr. Robert Moghim – CEO/Founder Colorado Pain Care
M.D. Disclaimer: The views expressed in this article are the personal views of Robert Moghim, M.D. and do not necessarily represent and are not intended to represent the views of the company or its employees. The information contained in this article does not constitute medical advice, nor does reading or accessing this information create a patient-provider relationship. Comments that you post will be shared with all visitors to this page. The comment feature is not governed by HIPAA and you should not post any of your private health information.



